Letter to Editor - Neuropsychiatry (2017) Volume 7, Issue 6
The Value of Gelfoam in Prevention of Recurrence Following Microvascular Decompression
- Corresponding Author:
- Jun Zhong, MD, PhD
Department of Neurosurgery, XinHua Hospital (The Cranial Nerve Disease Center of Shanghai)
Shanghai JiaoTong University School of Medicine
Shanghai 200092, China
Tel: 021-25078021
Fax: 021-25078025
Abstract
Trigeminal neuralgia, hemifacial spasm and glossopharyngsal neuralgia account for the majority of cranial nerve hyperexcitability disorders. As
vascular compression of the cranial nerve root has been believed to be the etiology, microvascular decompression (MVD) has nowadays become
the most effective remedy for these disorders.
Trigeminal neuralgia, hemifacial spasm and glossopharyngsal neuralgia account for the majority of cranial nerve hyperexcitability disorders [1]. As vascular compression of the cranial nerve root has been believed to be the etiology, microvascular decompression (MVD) has nowadays become the most effective remedy for these disorders [2]. Although about 90% of immediate postoperative cure might be achieved recently, a 6-30% of symptom recurrence has been reported [3]. The recurrence of those symptoms remains a challenge for neurosurgeons. The likelihood of recurrence is variable. There are many factors which can account for the recurrence following MVD, such as teflon granuloma formation, excessive teflon insert, improper and inadequate operative techniques, teflon adhesion and new vessels compression [4]. With experience of more than 10,000 MVDs [5], we believe that the adhesion of teflon felt is the main reason of the recurrence. Therefore, it should be the best if the neurovascular conflict could be separated without any external material insertion. Nevertheless, for most of the cases, it is the easy way to detach the offending vessel with soft telfon waddings. Accordingly, we suggest putting some moist gelatin sponges between the teflon felt and the nerve during the decompression procedure for those need teflon separation. (Figure 1). We think that placement of gelfoam between the nerve and the teflon has two functions: 1) as the size of gelatin sponge may enlarge more than 30 times in cerebrospinal fluid, it provides more rooms spontaneously between the teflon felt and the nerve, which make it easier to keep the offending vessel(s) away from the nerve; 2) as gelfoams are absorbed within four to six weeks, a clearance between the nerve and the teflon will be created, which avoids the teflon from adhering to the nerve and facilitates restoration of myelin sheath of the victim nerve root. With an incomplete statistical observation of our series, the relapse rate was approximately 4.7% in teflon-gelfoam group and 2.2% in teflon-alone group.
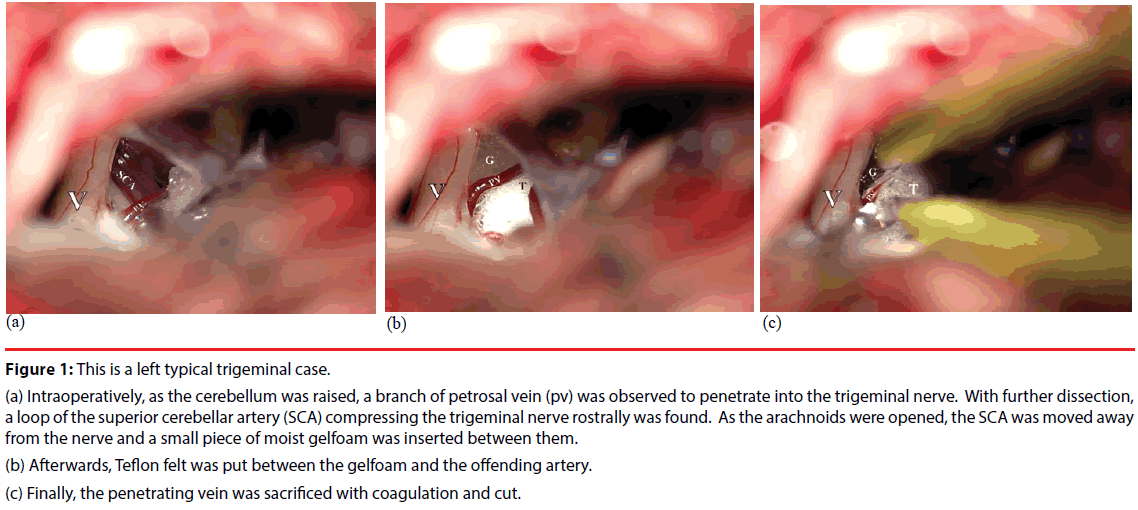
Figure 1: This is a left typical trigeminal case.
(a) Intraoperatively, as the cerebellum was raised, a branch of petrosal vein (pv) was observed to penetrate into the trigeminal nerve. With further dissection, a loop of the superior cerebellar artery (SCA) compressing the trigeminal nerve rostrally was found. As the arachnoids were opened, the SCA was moved away from the nerve and a small piece of moist gelfoam was inserted between them.
(b) Afterwards, Teflon felt was put between the gelfoam and the offending artery.
(c) Finally, the penetrating vein was sacrificed with coagulation and cut.
Acknowledgments
None
Funding
This work was supported by the China government under grant of National Natural Science Foundation (#81471317).
Conflicting Interest
None
References
- Xia L, Liu MX, Zhong J, et al. Fatal complications following microvascular decompression: could it be avoided and salvaged? Neurosurg. Rev 40(3), 389-396 (2016).
- Nash B, Carlson ML, Van Gompel JJ. Microvascular decompression for tinnitus: systematic review. J. Neurosurg 126(4), 1148-1157 (2017).
- Kondo A. Follow-up results of microvascular decompression in trigeminal neuralgia and hemifacial spasm. Neurosurgery 40 (1), 46-51; discussion 51-42 (1997).
- Matsushima T, Yamaguchi T, Inoue TK, et al. Recurrent trigeminal neuralgia after microvascular decompression using an interposing technique. Teflon felt adhesion and the sling retraction technique. Acta. Neurochir (Wien) 142 (5), 557-561 (2000).
- Zhong J, Zhu J, Sun H, et al. Microvascular decompression surgery: surgical principles and technical nuances based on 4000 cases. Neurol. Res 36(10), 882-893 (2014).