Case Report - (2021) Volume 11, Issue 1
What lies beneath a case of hypersexuality: rare presentation of progressive supranuclear palsy
- Corresponding Author:
- Ee Ying Hui
Dina. Geriatrics Medicine
Ng Teng Fong General Hospital, 1 Jurong East Street 21
Singapore 609606
E-mail: [email protected]
Abstract
During a hospitalisation for recurrent falls, a 78-year-old Chinese man was found to have inappropriate sexual behaviour. In the ward, he had pornographic material and inappropriately touched a female nurse. Further history from the family revealed that there was similar behaviour at home. After counselling the nurses, the patient was referred to the psychiatrist.
Keywords
Adolescents; Gender; Addiction to alcohol; Character accentuation; North of Russia
Case Report
In the 4 years prior to presentation, he sustained frequent falls of approximately 4 to 6 episodes yearly. He was also observed to have slow gait, dysarthria, and dysphagia. Having seen a neurologist for parkinsonism, he has been takinglow-dose levodopa/benserazide hydrochloride (Madopar®) combination 250mg daily. Nonetheless he still had postural instability, worsening dysphagia and falls.
Physical examination was significant for paucity of facial expression, bradykinesia, and dysarthria. Gait examination revealed freezing. His extra ocular movements, including saccades, were normal. Power was 5/5 (Medical Research Council grading) in all muscle groups.
A formal neuropsychological assessment did not find any significant deficits, other than poor visual attention and reduced information processing speed. The family later reported that, in the past year, he started to develop short term memory loss. Hence the initial diagnosis was mild cognitive impairment with frontal lobe symptoms. The psychiatrist started him on fluvoxamine but with limited improvement, henceswitched to escitalopram.
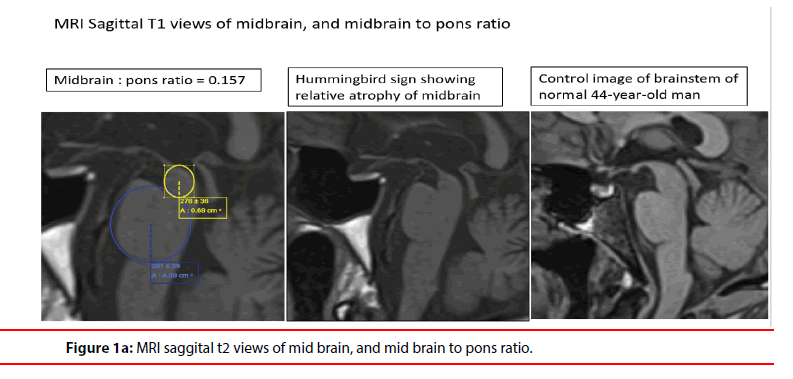
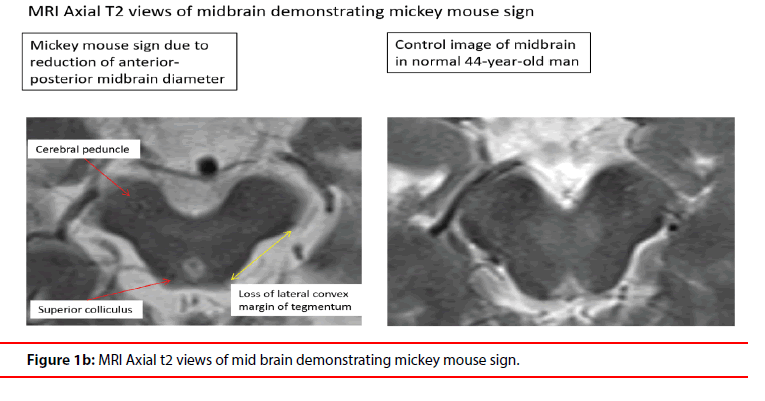
With normal full blood count, renal function, vitamin B12 levels, and thyroid function, his blood tests were largely unremarkable. A magnetic resonance imaging (MRI) of the brainperformed to evaluate his hypersexuality and cognitive impairment, revealed area of encephalomalacia in the left occipital lobe due to old infarct. Significantly, there was prominent midbrain atrophy with a midbrain to pons ratio of 0.157, its corresponding radiological “Hummingbird sign” (Figure 1a), and the “Mickey Mouse sign” (Figure 1b). There was no abnormality on the frontal or temporal lobe.
Both the clinical presentation and radiological features confirmed the diagnosis of progressive supranuclear palsy (PSP). A multidisciplinary team was involved for management, counselling, and advance care planning. Due to significant caregiver stress, the patient was institutionalised in a nursing home, with no recurrence of inappropriate sexual behaviour.
Discussion
PSP is a rare atypical Parkinsonian syndrome with an incidence of 1.4 per 100,000 to 4–7 per 100,000, and a mean survival of 6-10 years [1]. Our patient met most of the Neurological Disorders and Stroke and Society for Progressive Supranuclear Palsy (NINDS-SPSP) criteria of possible PSP, which includes gradually progressive disorder, onset after age 40 years and prominent postural instability with falls in the first year of onset [2]. He met supportive criteria such as poor levodopa responsiveness, early dysphagia, and dysarthria. However, he did not exhibit vertical supranuclear gaze palsy or slowing of vertical saccades, which are the clinical features that best discriminate PSP. Early presentation of PSP with neuropsychiatric symptoms is uncommon. Of these, patients tend to have apathy and executive impairment, while hypersexuality is rare [3].
Radiological signs, such as midbrain to pons ratio <0.52,which give 100% specificity for PSP diagnosis [4]. There is currently no effective treatment.Multidisciplinary interventions, including speech, occupational and physical therapy, should start early. Benefit of levodopa is minimal, while research into disease modifying therapies, with focus on agents with tau-active properties, is ongoing.
Although PSP is categorized as a movement disorder, patients with PSP can present with neuropsychiatric symptoms, which are atypical and pose diagnostic challenges. This case highlights the importance of considering PSP in a geriatric patient with hypersexuality. An accurate diagnosis aids in patient’s and family’s understanding of disease trajectory and prognosi.
Acknowledgments
There is no source of financial grants or other funding or any authors’ industrial links and affiliations.
Conflict of Interest
There is no financial support or relationships that may pose conflict of interest.
All authors have contributed significantly, had access to the data and a role in writing the manuscript; and are in agreement with the content of the manuscript.
References
- Golbe LI, Davis PH, Schoenberg BS. Prevalence and natural history of progressive supra neuclear palsy. Neurology 38(1), 1031–1034 (1988).
- Litvan I, Aged Y, Celne D et al. Clinical research criteria for the diagnosis of progressive supranuclear palsy (Steele–Richardson Olszewski syndrome): report of the NINDA-SPSP international workshop. Neurology 47(1), 1–9 (1996).
- Litvan I, Mega MS, Cummings JL. Neuropsychiatric aspects of progressive nuclear palsy. Neurology 47(1), 1184–1189 (1996).
- Stezin A, Lenka A, Jhunjhunwala K, et al. Advanced structural neuroimaging in progressive supranuclear palsy: Where do we stand? Parkinsonism Relat Disord 36:19–32 (2017).