Review Article - (2022) Volume 12, Issue 1
Neuropsychiatry and COVID-19: An Overview
Marcos Altable1*, Juan Moisés de la Serna2, Emilio Díaz-Moreno3, Alfonso Cruzado4, David Alvarez Montano5
1Department of Neurology, University Hospital Marqués de Valdecilla, Ceuta, Spain
2Department of Education, International University of La Rioja (UNIR), Madrid, Spain
3Department of Neuropsychology, Private Practice of Neuropsychology, HC Marbella, Ceuta, Spain
4Department of Psychologist at Ability, University Hospital Marqués de Valdecilla, Ceuta, Spain
5Department of Psychologist, Concentra Center, Ceuta, Spain
*Corresponding Author:Marcos Altable
Department of Neurology, University Hospital Marqués de Valdecilla, Ceuta, Spain
Email: [email protected]
Received date: 03-Jan-2022, Manuscript No. NPY-21-39853;
Editor assigned date: 05-Jan-2022, PreQC No. NPY-21-39853(PQ);
Reviewed date: 14-Jan-2022, QC No NPY-21-39853;
Revised date: 25-Jan-2022, Manuscript No. NPY-21-39853(R);
Published date: 31-Jan-2022, DOI: 10.37532/1758-2008.2022.12(1).614
Abstract
Most of studies that exist on the COVID-19 pandemic produced by the SARS-CoV-2 coronavirus, report neuropsychiatric symptoms only as part of the manifestation of the disease in its terminal phase. However, there are neuropsychiatric symptoms since the beginning of the disease. Several investigations have indicated a direct relationship between chronic diseases such as human immunodeficiency virus (HIV), tuberculosis, SARS, MERS, Ebola and SARS 2003 with mental disorders such as depression. Neuropsychiatric disorders can occur due to different mechanisms, such as cerebral hypoxia, cytokine storm due to exaggerated immune response and encephalitis due to direct brain infection. Nervous system involvement leads to poor prognosis of COVID-19.
Keywords
Neuropsychiatry, COVID-19, immunity, pathophysiology, cytokine neuroinvasion
Introduction
The Central Nervous System (CNS) is vulnerable to viruses [1]. Historically, past influenza pandemics have been associated with a post-infection increase in anxiety, insomnia, fatigue, depression, sociality, and delirium [2]. Furthermore, there is some debate as to whether the Spanish flu pandemic of 1918 was causally associated with encephalitis lethargic as a neurological consequence [3]. Other viruses end up reaching the brain, such as herpes virus, parvovirus, coronavirus, measles, and HIV, among others.
Most of studies that exist on the COVID-19 pandemic produced by the SARS-CoV-2 coronavirus, report neuropsychiatric symptoms only as part of the manifestation of the disease in its terminal phase. However, even if the infection is mild, moderate or severe, there are neuropsychiatric symptoms since the beginning of the disease.
Already in the advanced stages of the Severe Acute Respiratory Syndrome (SARS), different neuropsychiatric manifestations have been reported as a form of clinical expression of the course of infection, which could be a direct output of cerebral hypoxia due to respiratory failure, viral brain tissue infection or encephalitis, immune system reaction or cytokine storm or a combination of all these factors [4]. Neuropsychiatric manifestations include anxiety symptoms, panic attacks, depression, mental confusion, acute confessional syndrome, psychomotor excitement, psychosis, and even suicidal tendencies [5-8].
According to studies reviewed to date, neuropsychiatric symptoms can be divided into symptoms of the Central Nervous System (CNS), such as headache, dizziness, vertigo, altered consciousness, confusion, ataxia, acute cerebrovascular disease and seizures, Peripheral Nervous System (PNS) symptoms, such as anosmia, dyspepsia, neuralgia, and diarrhoea; and psychiatric symptoms such as apathy, depression, anorexia, psychosis, acute confessional syndrome, and agitation.
Several investigations have indicated a direct relationship between chronic diseases such as Human Immunodeficiency Virus (HIV) and tuberculosis, with mental disorders such as depression [9,10], in the general population [11,12]. Similarly, studies conducted during and after epidemics such as SARS and Ebola, found that there was a widespread behaviour induced by the hyperactive reaction among the general public [13,14]. In addition to this, various psychiatric disorders such as anxiety, depression, and Post Traumatic Stress Disorder (PTSD) were found mainly in survivors and healthcare workers [15-17].
Previous studies have reported adverse psychological reactions to the SARS outbreak among healthcare workers [18-21]. Studies showed that these health workers feared contagion and infection from their family, friends and colleagues, felt uncertainty and stigmatization, reported aversion to work, and high levels of stress, anxiety and symptoms of depression, that could have long-term psychological implications. Similar concerns are now emerging about mental health, psychological adjustment, and recovery for both the ill and the health workers who treat and care for patients with COVID-19. Besides, as the WHO has highlighted in its state of mental health, stigmatization and the scapegoat of affected people, including health professionals, is very common during epidemics [22,23]. Unfortunately, this trend continues to prevail during the current COVID-19 outbreak, as many people of Asian origin, explicitly Chinese, are victims of xenophobia and social stigmatization, with high levels of threats online and during public interactions [24].
Initially, the public emotional response to any pandemic is one of extreme fear and uncertainty that generally leads to negative social behaviours and can involve public mental health problems such as anxiety, insomnia, aggression, depression, frustration, and hysteria. Compared to previous studies related to SARS outbreaks, patients with COVID-19 (defined or suspected), and in quarantine, are more likely to suffer from loneliness, anger and frustration [25]. Similarly, another concern is that survivors and mental health professionals suffer from Post Traumatic Rhinitis Disorder (PTRD). In a study conducted at a Beijing hospital, quarantined health workers who worked in high-risk settings or had a family member with SARS reported a significantly higher level of post-traumatic stress symptoms compared to those without similar experiences [26,27]. Similarly, medical professionals who dealt with SARS patients or worked during the SARS outbreak also reported fear, anxiety, depression, and frustration. In comparison, health professionals working in COVID-19 quarantined units, lacking adequate protective measures and suffering the death of other physicians, may develop severe symptoms of post-traumatic stress disorder. For this reason, mental health professionals must apply therapies such as the stress adaptation model to reduce the level of high stress in this population [28].
Any situation of uncertainty can lead to alarmist behaviour, and with the influence of COVID-19, confinement, and the absence of adequate treatment for infectious disease, this situation has led the masses to moments of panic and anxiety [29]. Similarly, the obsession with contamination, which is persistent, for cleaning and the constant need for washing or sterilization is generally classified under obsessive-compulsive disorder [30]. Moreover, in the event of a pandemic caused by an infectious virus, this disorder can contribute to panic, resulting in disruption and impairment of the necessary daily activities of people. Mental health professionals and clinical psychologists must be alert to these impending problems and try to resolve them with the utmost care.
Pathophysiology
In many patients infected with SARS-CoV-2 and, even more, in those who develop moderate to severe respiratory failure, neuropsychiatric disorders can occur due to different mechanisms that can act concomitantly, such as cerebral hypoxia due to respiratory failure (mental confusion), cytokine storm due to exaggerated immune response (apathy, anorexia and muscular pain) and encephalitis due to direct brain infection (agitation and psychosis) [31,32]. The Angiotensin 2-Converting Enzyme (ACE2) has been identified as the functional receptor for SARS-CoV-2, which is present in multiple human organs, including the nervous system and the musculoskeletal system. The expression and distribution of ACE2 explain why SARS-CoV-2 can produce neuropsychiatric symptoms through direct and indirect mechanisms. Coronavirus encephalitis has also been confirmed, as in SARS-CoV and MERS-CoV. The researchers detected SARS-CoV nucleic acid in the cerebrospinal fluid of these patients and also brain tissue from the autopsies.
Another mechanism involved in many genetically predisposed patients is the cytokine storm generated by the interaction of the immune system with the virus, which, in addition to the systemic repercussion, primarily affects the nervous system. Cytokine storm resembles Macrophage Activation Syndrome (MAS), a severe condition that presents with hyper cytokinesis, fever, cytopenia and hyper ferritinemia, pulmonary involvement (including ARDS) and is associated with the severity of COVID-19 disease. It is characterized by an increase in interleukin (IL)-2, IL-7, granulocyte colony-stimulating factor, interferon-inducible protein 10-γ, monocyte chemo attractant protein 1, macrophage inflammatory protein 1-α and tumour necrosis factor-α [33].
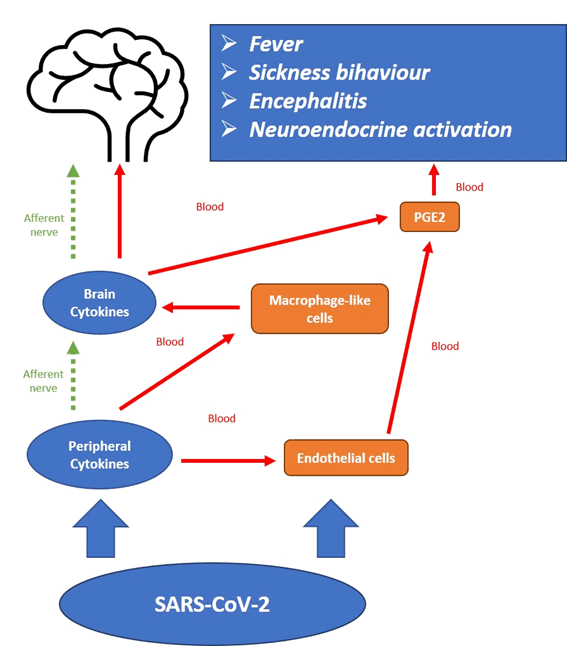
Brain cytokines produce behavioural changes (sickness behaviour) during the course of an illness or infection, manifesting depressive symptoms such as emotional hyper responsiveness, apathetic syndrome, anhedonia, hypoxia, weight loss, hypersomnia, alteration of the circadian rhythm, fatigue and chronic pain, psychomotor inhibition, demotivation, disinterest and alteration of higher mental functions [34-37]. Furthermore, it has been described a high level of this cytokines in blood and in the prefrontal cortex of teenage suicide victims [38]. It would appear that during acute coronavirus infection, immune hyper reactivity generates this behaviour syndrome with such variable neuropsychiatric symptoms. This is important since in terms of COVID-19 infection, beyond the typical symptoms of fever, cough and dyspnoea, the neuropsychiatric manifestations are added, which would be responsible for the symptoms of apathy, anorexia and muscular pain. These symptoms can go as far as the mental confusion, agitation, and psychosis that many patients may manifest even in initial stages, together with characteristic laboratory findings and pulmonary abnormalities. (Figure 1)
Figure 1 shows the mechanisms of action of cytokines on the brain. Pro inflammatory cytokines are released by immune cells at the periphery in response to SARS-CoV-2. Cytokines and virus act on macrophage-like cells in the brain, leading to the production of brain cytokines that diffuse by volume propagation into the parenchyma. Peripheral cytokines can reach out the brain by afferent nerves, resulting in the production of brain pro inflammatory cytokines by microglial cells. In both cases, the action of brain pro inflammatory cytokines can be mediated by prostaglandins (PGE2) that diffuse to brain targets or by activation of neural pathways within the brain, which enables the immune message to be transported far away from its site of origin. Prostaglandins can be synthesized only by endothelial cells of brain venules in response to circulating cytokines. Dotted arrows represent instances of neural transmission of the immune message from the periphery to the brain or within the brain itself [39].
Neurological complications
Today we know from the study of that from the beginning of the disease, 66% of hospitalized patients started with the most common symptoms like fever, dry cough, and dyspnea, but 34% started with neuropsychiatric symptoms such as dizziness (16%), headache (13%), dysgeusia (6%), and anosmia (5%). Furthermore, 40% of the total studied patients were severe, and 60% were non-severe, and within severe cases, 50% had neuropsychiatric symptoms. Within the non-severe group, 30% of cases presented neuropsychiatric symptoms. While within the group of severe cases with neuropsychiatric symptoms, these were due to stroke (5.7%), ischemic/haemorrhagic, altered consciousness (14.8%), and rhabdomyolysis (19.3%). Severe patients had a higher inflammatory response, including leucocytosis, neutrophilia, lymphopenia, increased CRP and higher D-dimer compared to non-severe cases, with D-dimer being an indicator of consumption coagulation pattern. Furthermore, severe patients had multiple organ involvement, such as liver failure (increased LDH, TGO, TGP), kidney failure (increased urea and creatinine), and rhabdomyolysis (increased CPK levels). In the laboratory findings of patients with more severe neuropsychiatric symptoms, lymphopenia, platelet count, and increased urea were found. For the non-severe subgroup, there were no significant differences in the laboratory findings of patients with and without neuropsychiatric symptoms. Patients with rhabdomyolysis had leucocytosis, lymphopenia, and increased CRP and D-dimer. Abnormalities were a manifestation of increased inflammatory response and impaired coagulation function. Additionally, it was observed that patients with rhabdomyolysis had multiple organ damage, including liver failure and kidney failure. For the severe group, patients with rhabdomyolysis had an increased inflammatory response (lymphopenia and increased CRP), liver failure, kidney, and rhabdomyolysis with increased CPK.
Likewise, 33% of the total of patients, severe and non-severe, had diverse neuropsychiatric manifestations. The severe patients were older (58 ± 10 years). The most frequent comorbidity in these cases was hypertension and, less frequently, they presented typical symptoms such as fever, cough and dyspnea. Furthermore, they were more likely to develop neuropsychiatric symptoms, especially mental confusion, agitation, and psychosis, and also acute cerebrovascular disease [40].
About 30% of the total of hospitalized patients had neuropsychiatric manifestations from the beginning of the infection, and the most severe or terminal patients probably develop neuropsychiatric symptoms in 45% as a manifestation of metabolic alteration or brain injury.
The interpretation of the data now is that, compared to non-severe patients with COVID-19, severe patients very frequently presented as predictors of mortality, elevated ferritin and IL-6 as biomarkers of viral inflammation and neuropsychiatric symptoms as alteration of consciousness, mental confusion, agitation, cerebrovascular disease, encephalitis, and rhabdomyolysis.
A newly published study classifies neurological damage in patients with COVID-19 in three stages. On Stage I the virus damage is limited to epithelial cells of nose and mouth and the main symptoms include transient loss of smell and taste. Subsequently, on Stage II the virus triggers a wave of inflammation, called cytokine storm, which begins in the lungs and travels in the blood vessels throughout all body organs. This cytokine storm leads to the formation of blood clots which cause cerebrovascular disease. Finally, on Stage III an explosive level of cytokine storm damages the Blood-Brain Barrier (BBB) and as a result, blood content, inflammatory markers, and virus particles invade the brain and patients develop seizures, confusion, coma, orencephalopathy [41]. (Table 1)
| N% | |||
|---|---|---|---|
| Total | Severe | Nonsevere | |
| COMORBILITIES | |||
| Any | 83 (38.8) | 42 (47.7) | 41 (32.5) |
| Hypertension | 51 (23.8) | 32 (36.4) | 19 (15.1) |
| Diabetes | 30 (14.0) | 15 (17.0) | 15 (11.9) |
| Cardia/Cerebrovascular disease | 15 (7.0) | 7 (8.0) | 8 (6.3) |
| Malignancy | 13 (6.1) | 5 (5.7) | 8 (6.3) |
| Chronic kidney disease | 6 (2.8) | 2 (2.3) | 4 (3.2) |
| TYPICAL SYMPTOMS | |||
| Fever | 132 (61.7) | 40 (45.5) | 92 (73.0) |
| Cough | 107 (50.0) | 30 (34.1) | 77 (61.1) |
| Anorexia | 68 (31.8) | 21 (23.9) | 47 (37.3) |
| Diarrhea | 41 (19.2) | 13 (14.8) | 28 (22.2) |
| Throat pain | 31 (14.5) | 10 (11.4) | 21 (16.7) |
| Abdominal pain | 10 (4.7) | 6 (6.8) | 4 (3.2) |
| NERVOUS SYSTEM SYMPTOMS | |||
| Any | 78 (36.4) | 40 (45.5) | 38 (30.2) |
| CNS | 53 (24.8) | 27 (30.7) | 26 (20.6) |
| Dizziness | 36 (16.8) | 17 (19.3) | 19 (15.1) |
| Headache | 28 (13.1) | 15 (17.0) | 13 (10.3) |
| Impaired consciousness | 16 (7.5) | 13 (14.8) | 3 (2.4) |
| ACD | 6 (2.8) | 5 (5.7) | 1 (0.8) |
| Ataxia | 1 (0.5) | 1 (1.1) | 0 NA |
| Seizure | 1 (0.5) | 1 (1.1) | 0 Na |
| PNS | 19 (8.9) | 7 (8.0) | 12 (9.5) |
| Impairment | |||
| Taste | 12 (5.6) | 3 (3.4) | 9 (7.1) |
| Smell | 11 (5.1) | 3 (3.4) | 8 (6.3) |
| Vision | 3 (1.4) | 2 (2.3) | 1 (0.8) |
| Nerve pain | 5 (2.3) | 4 (4.5) | 1 (0.8) |
| SKELETAL MUSCLE INJURY | 23 (10.7) | 17 (19.3) | 6 (4.8) |
| ONSET OF SYMPTOMS(*) | |||
| CNS | |||
| Dizziness | 1 (1-30) | 1 (1-30) | 1 (1-14) |
| Headache | 1 (1-14) | 1 (1-3) | 3 (1-14) |
| Impaired consciousness | 8 (1-25) | 10 (1-25) | 1 (1-3) |
| Acute CVD | 9 (1-18) | 10 (1-18) | 1 (1) |
| Ataxia | 2 (2) | 2 (2) NA | NA |
| Seizure | 2 (2) | 2 (2) NA | NA |
| PNS | |||
| Impairment | |||
| Taste | 2 (1-5) | 3 (1-3) 2 (1-5) | NA |
| Smell | 2 (1-5) | 1 (1-4) 2 (1-5) | NA |
| Vision | 2 (1-3) | 3 (2-3) 1 (1) | NA |
| Nerve pain | 1 (1-1) | 1(1-1) 1 (1) | NA |
| SKELETAL MUSCLE INJURY | 1 (1-11) | 1 (1-11) 1 (1-6) | NA |
Table 1: An explosive level of cytokine storm damages the Blood-brain barrier
With all of the above, the new clinical information on COVID-19 would help to take into account the participation of neuropsychiatric manifestations, especially in patients with Severe COVID-19, due to the rapid clinical deterioration or worsening that could be more related frequently with the appearance of mental confusion, confusional syndrome, agitation and strokes. Increasing the mortality rate. Likewise, during the epidemic period of COVID-19, when treating patients with neuropsychiatric manifestations, SARS-CoV-2 infection should be considered as a first-line differential diagnosis to avoid late or misdiagnosis and to prevent transmission.
Neuropsychiatric symptoms were the main form of manifestation of altered brain metabolism or neurological injury in reported COVID-19 patients. The pathophysiological mechanism could be the invasion of the Central Nervous System (CNS) by SARS-CoV-2, similar to the SARS and MERS viruses. Like other respiratory viruses, SARS-COV-2 can enter the CNS via the hematogenous or retrograde neuronal pathway (since many patients presented anosmia or dysgeusia in initial stages). Lymphopenia has also been detected in patients with neuropsychiatric symptoms. This phenomenon may be indicative of immunosuppression in COVID-19 patients with neuropsychiatric symptoms, especially in severe subgroup.
On the other hand, severe cases have also been found to have high D-dimer suggestive of a hypercoagulable state. This may be the reason why seriously ill patients are more likely to develop cerebrovascular disease.
In summary, SARS-CoV-2 can infect the nervous system, the skeletal muscle and the respiratory tract. In those with severe infection, neuropsychiatric involvement is more likely, including altered consciousness, mental confusion, agitation, acute cerebrovascular disease, and rhabdomyolysis. Nervous system involvement leads to poor prognosis due to greater hemodynamic instability, worsening clinical conditions and increased mortality.
References
- Xia H, Lazartigues E. Angiotensin-converting enzyme 2: Central regulator for cardiovascular function. Curr Hypertens Rep 12(3), 170-175 (2010). [Crossref] [Google Scholar] [Indexed]
- Honigsbaum M. An inexpressible dread: Psychoses of influenza at fin-de-siècle. Lancet 381(9871), 988-989 (2013). [Crossref] [Google Scholar] [Indexed]
- Hoffman LA, Vilensky JA. Encephalitis lethargica: 100 years after the epidemic. Brain 140(8), 2246-2251 (2017). [Crossref] [Google Scholar] [Indexed]
- Liu TB, Chen XY, Miao GD, et al. Recommendations on diagnostic criteria and prevention of SARS-related mental disorders. J Clin Psychol Med 13(3), 188-191 (2003). [Crossref] [Google Scholar] [Indexed]
- Ibrahim E, Ibrahim NE. Review of published systematic reviews and meta-analyses on COVID-19. MedRxiv 6(3), 20121137 (2020). [Crossref] [Google Scholar] [Indexed]
- Jain V, Jain M, Saluja SS, et al. Coronavirus disease: A review. j. innov 7(6), 2348-7689 (2020). [Crossref] [Google Scholar] [Indexed]
- Katta M, Rapaka S, Adireddi R, et al. A preliminary review on novel coronavirus disease: COVID-19. Bentham Science 1(1), 90-97 (2020). [Crossref] [Google Scholar]
- Tejaswi JKD. Overview on COVID 19: A review. Indian J Pediatr 87(4), 281–286 (2020). [Crossref] [Google Scholar] [Indexed]
- Gale SD, B errett AN, Erickson LD, et al. Association between virus exposure and depression in US adults. Psychiatry Res 261, 73-79 (2018). [Crossref] [Google Scholar] [Indexed]
- Mason BW, Lyons RA. Acute psychological effects of suspected bioterrorism. J Epidemiol Community Health 57(5), 353-354 (2003). [Crossref] [Google Scholar] [Indexed]
- Kuan V, Denaxas S, Gonzalez IA, et al. A chronological map of 308 physical and mental health conditions from 4 million individuals in the english national health service. Lancet Digit Health 1(2), e63-e77 (2019). [Crossref] [Google Scholar] [Indexed]
- Van Den Heuvel L, Chishinga N, Kinyanda E, et al. Frequency and correlates of anxiety and mood disorders among TB and HIV infected zambians. AIDS Care 25(12), 1527-1535 (2013). [Crossref] [Google Scholar] [Indexed]
- Person B, Sy F, Holton K, et al. Fear and stigma: The epidemic within the SARS outbreak. Emerg Infect Dis 10(2), 358-363 (2004). [Crossref] [Google Scholar] [Indexed]
- Shultz JM, Cooper JL, Baingana F, et al. The role of fear related behaviors in the 2013-2016 west africa ebola virus disease outbreak. Curr Psychiatry Rep 8(11), 104 (2016). [Crossref] [Google Scholar] [Indexed]
- Blakey SM, Kirby AC, McClure KE, et al. Posttraumatic safety behaviors: characteristics and associations with symptom severity in two samples. Traumatology 26(1), 74-83 (2019). [Crossref] [Google Scholar] [Indexed]
- Gardner PJ, Moallef P. Psychological impact on SARS survivors: Critical review of the english language literature. Canadian Psychology 56(1), 123-135 (2015). [Crossref] [Google Scholar] [Indexed]
- Mak IWC, Chu CM, Pan PC, et al. Long-term psychiatric morbidities among SARS survivors. Gen Hosp Psychiatry 31(4), 318-326 (2009). [Crossref] [Google Scholar] [Indexed]
- Arabi YM, Balkhy HH, Hayden FG, et al. Middle east respiratory syndrome. NEJM 376(6), 584-594 (2017). [Crossref] [Google Scholar] [Indexed]
- Hamming I, Timens W, Bulthuis MLC, et al. Tissue distribution of ACE2 protein, the functional receptor for SARS coronavirus. A first step in understanding SARS pathogenesis. J Pathol 203(2), 631-637 (2004). [Crossref] [Google Scholar] [Indexed]
- https://www.who.int/emergencies/mers-cov/en/
- Wu P, Fang Y, Guan Z, et al. The psychological impact of the SARS epidemic on hospital employees in china: Exposure, risk perception, and altruistic acceptance of risk. Can J Psychiatry 54(5), 302–311 (2009). [Crossref] [Google Scholar] [Indexed]
- Rubin GJ, Wessely S. The psychological effects of quarantining a city. BMJ 368, 313 (2020). [Crossref] [Google Scholar] [Indexed]
- Shigemura J, Ursano RJ, Morganstein JC, et al. Public responses to the novel 2019 coronavirus (2019-nCoV) in Japan: Mental health consequences and target populations. Psychiatry Clin Neurosci 74(4), 281-282 (2020). [Crossref] [Google Scholar] [Indexed]
- https://www.who.int/docs/default-source/coronaviruse/mental-health-considerations.pdf
- Xiang YT, Yang Y, Li W, et al. Timely mental health care for the 2019 novel coronavirus outbreak is urgently needed. Lancet Psychiatry 7(3), 228-229 (2020). [Crossref] [Google Scholar] [Indexed]
- Yi Y, Lagniton PNP, Ye S, et al. COVID-19: What has been learned and to be learned about the novel coronavirus disease. Int J Biol Sci 16(10), 1753-1766 (2020). [Crossref] [Google Scholar] [Indexed]
- Guan W, Kaiser, Ni Z, et al. Clinical characteristics of 2019 novel coronavirus infection in China. NEJM 2(6), 20020974 (2020). [Crossref] [Google Scholar]
- Folkman S, Greer S. Promoting psychological well-being in the face of serious illness: When theory, research and practice inform each other. Psychooncolog 9(1), 11-19 (2000). [Crossref] [Google Scholar] [Indexed]
- Soofi M, Najafi F, Karami MB. Using insights from behavioral economics to mitigate the spread of COVID-19. Health Econ. Health Policy 18, 345-350 (2020). [Crossref] [Google Scholar] [Indexed]
- Williams MT, Mugno B, Franklin M, et al. Symptom dimensions in obsessive-compulsive disorder: Phenomenology and treatment outcomes with exposure and ritual prevention. Psychopathology 46(6), 365-76 (2013). [Crossref] [Google Scholar] [Indexed]
- Ahmed SF, Quadeer AA, McKay MR. Preliminary identification of potential vaccine targets for the COVID-19 coronavirus (SARS-CoV-2) based on SARS-CoV immunological studies. Viruses 12(3), 254 (2020). [Crossref] [Google Scholar] [Indexed]
- Mao L, Jin H, Wang M, et al. Neurologic manifestations of hospitalized patients with coronavirus disease 2019 in wuhan, china. JAMA Neurol 77(6) , 683-690 (2020). [Crossref] [Google Scholar] [Indexed]
- Mehta P, McAuley DF, Brown M, et al. COVID-19: Consider cytokine storm syndromes and immuno suppression. Lancet 395(10229), 1033-1034 (2020). [Crossref] [Google Scholar] [Indexed]
- Dantzer R, Connor JOC, Freund GG, et al. From inflammation to sickness and depression: When the immune system subjugates the brain. Nat Rev Neurosci 9(1), 46-56 (2008). [Crossref] [Google Scholar] [Indexed]
- Debnath M, Berk M, Maes M. Changing dynamics of psychoneuroimmunology during COVID-19 pandemic. Brain Behav Immun Health 5, 100096 (2020). [Crossref] [Google Scholar] [Indexed]
- Miller AH. Mechanisms of cytokine-induced behavioural changes: Psycho neuro immunology at the translational interface. Brain Behav Immun Health 23(2), 149-158 (2009). [Crossref] [Google Scholar] [Indexed]
- Raison CL, Capuron L, Miller AH. Cytokines sing the blues: Inflammation and the pathogenesis of depression. Trends Immunol 27(1), 24-31(2006). [Crossref] [Google Scholar] [Indexed]
- Pandey GN, Rizavi HS, Ren X, et al. Proinflammatory cytokines in the prefrontal cortex of teenage suicide victims. J Psychiatr Res 46(1), 57-63 (2012). [Crossref] [Google Scholar] [Indexed]
- Dantzer R. Cytokine, sickness behaviour, and depression. Immunol Allergy Clin North Am 29(2), 247-264 (2006). [Crossref] [Google Scholar] [Indexed]
- Altable M, De La Serna JM. Cerebrovascular disease in COVID-19: Is there a higher risk of stroke? Brain Behav Immun Health 6, 100092 (2020). [Crossref] [Google Scholar] [Indexed]
- Fotuhi M, Mian A, Meysami S, et al. Neurobiology of COVID-19. J Alzheimers Dis 76(1), 3-19 (2020). [Crossref] [Google Scholar] [Indexed]