Case Report - (2018) Volume 8, Issue 5
Henoch-Scholein Purpura Related to Fluoxetine Medication in a Child
- Corresponding Author:
- Ying-Hsiang Chuo
Department of Pediatrics, Fu-Jen Catholic University Hospital, New Taipei, Taiwan
Tel: +886-2-85128867
Abstract
Background
Fluoxetine, one kind of selective serotonin reuptake inhibitors (SSRI), has rarely been reported to be related to vasculitis in adults.
Methods
Herein we present a boy who developed Henoch–Schönlein purpura (HSP) during treatment with fluoxetine.
Results
This 8-year-old boy suffered from depression about 3 months after he entered a new school. He visited a psychiatric clinic and fluoxetine was prescribed. The response was good and he went back to school smoothly. Sixth weeks later, he developed purpuric rash over bilateral lower extremities which extended to buttock and hands in two days. Mild painful swelling over left ankle was also noted when he was admitted. The investigations were normal including complete blood cell & platelet count, blood biochemistry, liver function tests, prothrombin time, partial thromboplastin time, serum immunoglobulin A and fibrinogen level. Yet D-dimer level was elevated to 8927 μg/dl (normalï¼Âœ500), consistent with vasculitis. The diagnosis of HSP was made and fluoxetine ceased. Treatment was given with Prednisolone and Ranitidine, after which the purpura resolved in one week.
Conclusions
HSP related to fluoxetine medication has rarely been reported in the young adults. Our case may attribute to be the youngest one who receives fluoxetine therapy and give us an example of the potential adverse effect of fluoxetine to the children.
Keywords
Henoch-Scholein Purpura, Vasculitis
Introduction
Henoch–Schönlein purpura has been a common systemic vasculitis in children. It usually presents with a triad of purpura, arthritis/arthralgia, and abdominal pain or renal disease (tetrad) [1]. This disease is characterized by the deposition of immunoglobulin IgA immune complexes presented in the vessel walls of arterioles, capillaries and venules. HSP belongs to the group of nongranulomatous, predominantly small vessel vasculitides, according to the new classification of childhood vasculitis [2].
HSP patients frequently have a preceding trigger of respiratory tract infection, with the common pathogens of streptococcus, staphylococcus, virus and mycoplasma [3,4]. Vaccination is another trigger factor [5]. The association between drug and HSP has also been implicated in several reports [6-8]. Herein we present a boy who developed HSP during treatment with fluoxetine.
Case Report
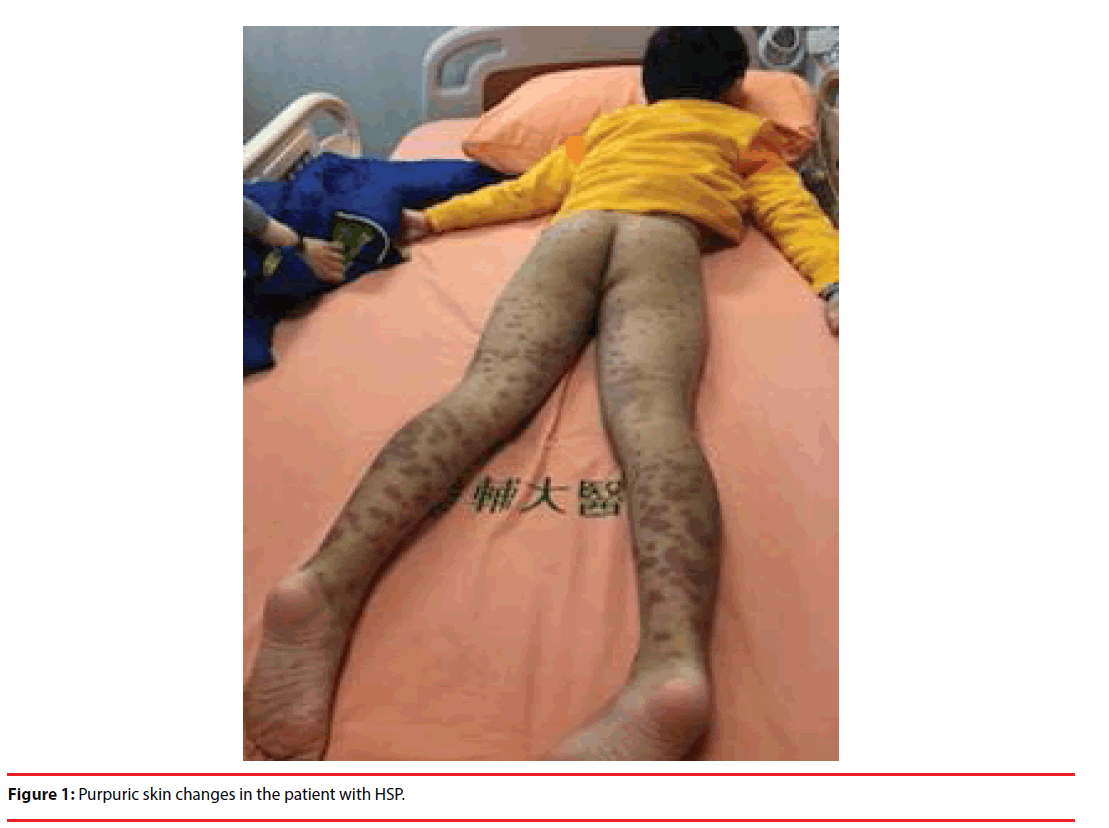
This 8-year-old boy suffered from depression about 3 months after he entered a new school. He visited a psychiatric clinic and fluoxetine was prescribed. The response was good and he went back to school smoothly. Sixth weeks later, he developed purpuric rash over bilateral lower extremities which extended to buttock and hands in two days (Figure 1). Most of the purpuras were slightly palpable without blanching when pressed. Mild painful swelling over left ankle was also noted when he was admitted. No abdominal pain was felt at all. The other physical findings were non-contributory. The investigations were normal including complete blood cell & platelet count, blood biochemistry, liver function tests, prothrombin time and partial thromboplastin time. Serum immunoglobulin A was 297 mg/ dl (normal range: 70-400) and fibrinogen level 237mg/dl (normal range: 180-350). Serum antinuclear antibody was negative. The stool & urine analysis showed normal findings. Yet D-dimer level was elevated to 8927 μg/dl (normal<500), consistent with vasculitis. The diagnosis of HSP was made. According to the Adverse Drug Reaction (ADR) Probability Scale (Naranjo Scale) [9], the ADR probability score was 4 (possible association) and fluoxetine was stopped. Treatment was given with Prednisolone and Ranitidine, after which the purpura resolved in one week. The patient eventually outgrew depression and skin rash without further medication during the following months.
Discussion
The association between drugs and HSP has been reported in many studies, though the role of drug in the pathogenesis of HSP is uncertain. Among the drugs reported to be related to the development of HSP, there have been antibiotics [10], anti-emetics [11], analgesia [12], anticoagulants [13], anticonvulsants [14], TNF-α inhibitors [15] for autoimmune diseases, anti-hypertensive [16], anti-neoplastic [17] and anti-arrhythmic agents [18], as well as antidepressants [19].
Many antidepressants may induce a variety of skin reactions [19,20]. The common and less risk drug reactions contain drug-induced urticaria, maculopapular rash, photo-sensitivity and fixed drug reactions. Besides, there are severe skin complications associated with antidepressants, reported as erythema multiforme, Stevens- Johnson syndrome, toxic epidermal necrolysis and drug hypersensitivity vasculitis including HSP. There have been few reports [19,20], mostly from adult patients, describing on vasculitis related to selective serotonin reuptake inhibitors (SSRI). Fluoxetine, one kind of SSRI, has rarely been reported to be related to vasculitis in adolescents and young adults. In children, there was only one ever reported on a 15 years old boy, as searched in the literature [21-23].
He had fluoxetine medication for 1 week, due to depression from his father’s death. He then developed generalized purpuric rash over lower legs associated with ankle and knee pain. The laboratory investigations showed almost normal except high level of D-dimer (3468 μg/dl) and mild proteinuria. The Naranjo scale was 6, which belonged to a probable causative association. Our case has the similar clinical picture, yet may attribute to be the youngest one who receives fluoxetine therapy. It could give us an example about the potential adverse effect of fluoxetine to the children.
References
- Trnka P. Henoch-Schönlein purpura in children. J. Paediatr. Child. Health 49(12), 995- 1003 (2013).
- Ozen S, Ruperto N, Dillon MJ, et al. EULAR/ PReS endorsed consensus criteria for the classification of childhood vasculitides. Ann. Rheum.Dis 65(7), 936-941 (2006).
- Weiss PF, Klink AJ, Luan X, et al. Temporal association of Streptococcus, Staphylococcus, and parainfluanza pediatric hospitalizations and hospitalized cases of Henoch-Schönlein purpura. J. Rheumatol 37(12), 2587-2594 (2010).
- Kano Y, Mitsuyama Y, Hirahara K, et al. Mycoplasma pneumoniae infection-induced erythema nodosum, anaphylactoid purpura, and acute urticaria in 3 people in a single family. J. Am. Acad. Dermatol 57(1), S33-S35 (2007).
- Watanabe T. Henoch-Schönlein purpura following influenza vaccinations during the pandemic of influenza A (H1N1). Pediatr. Nephrol 26(5), 795-798 (2011).
- Rolle AS, Zimmermann B, Poon SH. Etanercept-induced Henoch-Schönlein purpura in a patient with ankylosing spondylitis. J. Clin. Rheumatol 9(2), 90-93 (2013).
- Conti-Beltraminelli M, Pagani O, Ballerini G, et al. Henoch-Schönlein purpura (HSP) during treatment with anastrozole. Ann. Oncol 18(1), 131-134 (2006).
- Borrás-Blasco J, Enriquez R, Amoros F, et al. Henoch-Schönlein purpura associated with clarithromycin. Case report and review of literature. Int. J. Clin. Pharmacol.Ther 41(5):213- 216 (2003).
- Naranjo CA, Busto U, Sellers EM, et al. A method for estimating the probability of adverse drug reactions. Clin. Pharmacol. Ther 30(2), 239-245 (1981).
- Wakefield IR, Hunter DA. Antibiotic associated Henoch-Schonlein purpura syndrome. Br. J. Clin. Pract 42(12), 525-526 (1988).
- Upputuri S, Prasad S. Metoclopramideinduced delayed non-thrombocytopenic purpuric rash. Clin. Drug. Investig 6(12),745- 747 (2006).
- Santoro D, Stella M, Castellino S. Henoch- Schönlein purpura associated with acetaminophen and codeine. Clin. Nephrol 66(2):131-134 (2006).
- Borrás-Blasco J, Girona E, Navarro-Ruiz A, et al. Acenocoumarol-induced Henoch-Schönlein purpura. Ann. Pharmacother 38(2), 261-264 (2004).
- Kaneko K, Igarashi J, Suzuki Y, Niijima S, Ishimoto K, Yabuta K. Carbamazepineinduced thrombocytopenia and leucopenia complicated by Henoch-Schönlein purpura symptoms. Eur. J. Pediatr 152(9), 769-770 (1993).
- Asahina A, Ohshima N, Nakayama H, et al. Henoch-Schönlein purpura in a patient with rheumatoid arthritis receiving etanercept. Eur. J. Dermatol 20(4), 521-522 (2010).
- Moots RJ, Keeling PJ, Morgan SH. Adult Schönlein-Henoch purpura after enalapril. Lancet 340(8814), 04-305 (1992).
- Aktas B, Topcuoglu P, Kurt OK, et al. Severe Henoch-Schönlein purpura induced by cytarabine. Ann. Pharmacother 43(4), 792-793 (2009).
- Kuo M, Winiarski N, Garella S. Nonthrombocytopenic purpura associated sequentially with nifedipine and diltiazem. Ann. Pharmacother 26(9), 1089-1090 (1992).
- Margolese HC, Chouinard G, Beauclair L, Rubino M. Cutaneous vasculitis induced by paroxetine. Am. J. Psychiatry 158(3), 497-497 (2001).
- Herstowska M, Komorowska O, Cubata WJ, et al. Severe skin complications in patients treated with antidepressants: a literature review. Postepy. Dermatol. Alergol 31(2), 92-97 (2014).
- Welsh JP, Cusack CA, Ko C. Urticarial vasculitis secondary to paroxetine. J. Drugs. Dermatol 5(10), 1012-1014 (2006).
- Cederberg J, Knight S, Svenson S, et al. Itch and skin rash from chocolate during fluoxetine and sertraline treatment: case report. BMC Psychiatry 4, 36 (2004).
- Süleyman A, Kurt FS, Soyata AZ, et al. Henoch-Schönlein purpura during treatment with fluoxetine. J. Child. Adolescent. Psychopharmacol 26(7), 651-651 (2016).